Pulmonary Embolism: Signs, Emergency Steps, Diagnosis, and Prevention
A pulmonary embolism (PE) is a blood clot that blocks an artery in the lungs. It can come on fast and feels scary — sudden shortness of breath, chest pain, a cough with blood, fainting, or a racing heartbeat. Some people get subtle symptoms; others get a life‑threatening event. Knowing the red flags and what to do right away makes a big difference.
PE usually starts as a deep vein thrombosis (DVT) in the leg. Pieces of that clot can break off and travel to the lungs. Risk factors include recent surgery or trauma, long bed rest or flights, cancer, pregnancy, hormone therapy or birth control, obesity, smoking, and genetic clotting disorders. Older age and history of blood clots raise the risk too.
How PE is diagnosed and treated
If someone looks unwell with sudden breathlessness or chest pain, call emergency services immediately. At the hospital, providers check oxygen levels, heart rate, blood pressure, and do an ECG. Common tests include a D‑dimer blood test (good for ruling out PE in low‑risk cases), CT pulmonary angiography (the best test to see clots in the lungs), and a leg ultrasound to find a DVT. A V/Q scan is used when CT isn’t possible, such as with kidney problems or pregnancy.
Treatment starts quickly. Most patients receive anticoagulants (blood thinners) like low molecular weight heparin, direct oral anticoagulants (rivaroxaban, apixaban), or warfarin. These stop the clot from growing and help the body dissolve it. In severe cases with unstable blood pressure or right‑heart strain, doctors may use clot‑busting drugs (thrombolysis) or a catheter procedure to remove the clot. An IVC filter is an option when anticoagulation isn’t possible.
How long you stay on blood thinners depends on why the clot happened. A clot after surgery or a one‑time event often means 3 months of treatment. Unexplained clots, cancer, or repeated clots can mean longer or even indefinite therapy. Your doctor will weigh bleeding risk and recurrence risk to decide.
Reduce your risk and what to do now
Simple steps cut risk: move early after surgery, avoid long periods sitting, drink fluids, and wear compression stockings on long flights. If your doctor prescribes blood thinners after surgery or hospital stays, take them exactly as directed. During flights, stand and walk every hour, flex your ankles, and consider graduated compression socks if you have risk factors.
Suspect a PE? Sit up, stay calm, and call emergency services — don’t drive yourself if you’re short of breath or lightheaded. After treatment, follow up with a specialist, review the cause, and discuss lifestyle changes like quitting smoking and weight control. With quick care and the right prevention, most people recover well and can lower the chance of another clot.
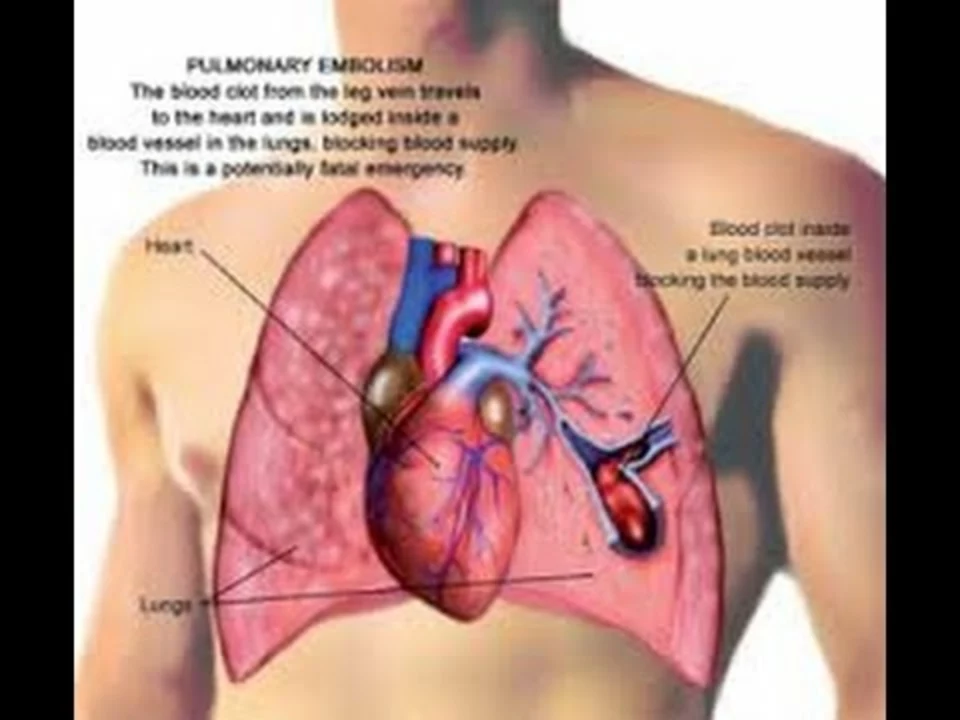
How Pulmonary Embolism Affects Your Heart and Lungs
As someone who recently learned about pulmonary embolism, I felt it was important to share how this condition affects our heart and lungs. A pulmonary embolism occurs when a blood clot blocks one of the arteries in the lungs, leading to reduced blood flow and potential damage. It puts a significant strain on the heart, as it has to work harder to pump blood through the blocked artery. This can ultimately cause heart failure and even death. It's crucial to be aware of the warning signs and seek immediate medical attention if you suspect a pulmonary embolism.
read more
