Colonoscopy is widely recognized as the gold standard for detecting and preventing colorectal cancer. However, the most powerful tool in your doctor's arsenal is only effective if you get the preparation right.
You might view the colonoscopy preparationprotocol as an annoying hurdle before the actual medical appointment. But in reality, the preparation phase determines the entire success of the procedure. If your colon is not perfectly clean, your doctor literally cannot see the lining clearly. This oversight leads to missed polyps-precancerous growths that cause the majority of colorectal cancer cases. Recent data indicates that incomplete cleansing happens in roughly 25% of exams. When this occurs, doctors miss potential issues in nearly half of those cases. You don't want to fall into that statistic.
The Critical Link Between Prep Quality and Cancer Prevention
Before diving into the schedule, it helps to understand what is actually at stake. Colorectal cancerrankings show it remains one of the top causes of cancer deaths worldwide. The silver lining is that it is almost entirely preventable through screening. The process works like this: a doctor looks for polyps during the exam. If they find a polyp, they remove it. If they miss it because of leftover waste, that polyp stays there to grow. Studies referenced by major health institutions suggest that excellent preparation increases the detection rate of these polyps by up to 25% compared to poor preparation.
Medical professionals track a metric called the Adenoma Detection Rate or ADR. This measures how many patients have polyps found during their exam. Higher rates correlate directly with lower risks of developing cancer later. Your behavior in the days leading up to the appointment impacts this number. It isn't just about comfort; it is about giving your healthcare provider the best possible view of your internal health.
Your Three-Day Preparation Timeline
Successful preparation follows a strict chronological order. Rushing this process or starting too late often results in a canceled procedure. Most experts recommend beginning specific changes 48 to 72 hours before your scheduled time. Here is the logical progression you need to follow.
| Time Before Procedure | Action Required | Key Focus |
|---|---|---|
| 72-48 Hours | Low-fiber diet begins | Reduce bulk in digestive system |
| 24 Hours | Clear liquid diet only | No solid food, avoid colors |
| 12-18 Hours | Bowel cleansing medication | Split-dose intake strategy |
| 3 Hours | Stop all intake | Fasting window starts |
Navigating Dietary Restrictions Without Stress
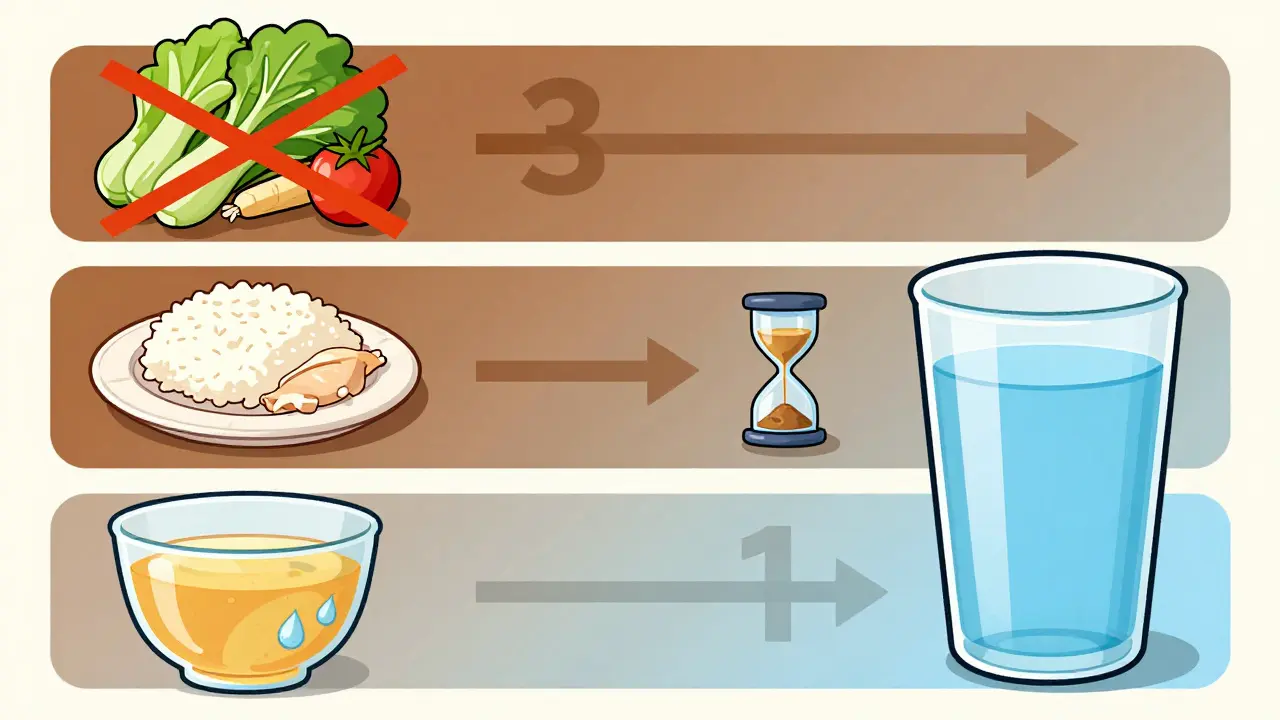
The diet modification begins three days prior. You need to switch to a low-fiber regimen immediately. Fiber adds bulk to stool that laxatives cannot move efficiently. You should eliminate raw fruits, nuts, seeds, and whole grains. Instead, opt for easily digestible options like steamed vegetables, white rice, pasta, plain chicken, and eggs. This transition reduces the residue load before you even start drinking the cleansing solution.
The day before the exam marks a significant shift. You move to a clear liquid diet. This means nothing with pulp, nothing opaque, and definitely no solids. Permitted liquids include water, black coffee, tea without milk, broth, and specific juices like apple or white grape. Crucially, you must strictly avoid red, purple, or orange liquids. These pigments can stain the colon lining. To the endoscopist's eye, that stain looks exactly like fresh blood or tissue irregularities. Consuming red Jell-O or berry juice could lead to unnecessary biopsies or a failed exam.
Mastering the Laxative Solution
The medication regimen is the most challenging part for most people. Current best practices favor a split-dose protocol rather than taking the entire volume the night before. You will drink half the solution in the evening, typically finishing around 6 PM. Then, you finish the remaining portion 4 to 6 hours before your appointment time. This timing ensures your colon is flushed clean right before the scope enters.
Tolerability is the main complaint patients report. Research shows that chilling the solution makes it significantly more palatable. Drinking it cold through a straw bypasses many taste buds on the tongue. Some formulations allow you to mix powder with a flavored beverage like Gatorade, provided the color is yellow or light green. You must stay hydrated alongside this process. Aim for eight ounces of water per hour while you are awake during the prep phase. Dehydration leads to dizziness and headaches, which can make you feel sick faster and stop you from finishing the dose.
Common Mistakes That Ruin Cleanliness
Even with the best intentions, specific errors occur frequently. Non-adherence to the written instructions is the primary reason for suboptimal cleansing. Many patients think "close enough" counts, but it does not. Taking constipating medications is another major pitfall. Iron supplements and certain painkillers slow down bowel movement. Unless your doctor tells you otherwise, stop iron supplements at least three days before the procedure.
Another frequent error involves the fasting window. You must stop eating and drinking anything solid three hours before the procedure begins. If you sneak a sip of water too close to arrival, safety protocols will require cancellation. This puts anesthesia at risk and delays your screening. Finally, hydration plays a huge role in success. About 15% of patients fail because they do not drink enough water with the prep, resulting in concentrated waste that does not flush cleanly.

Practical Comfort Strategies During Prep
Making the physical experience manageable requires some preparation of your own. Stock your bathroom with soft toilet paper and unscented wet wipes to prevent irritation, which can become significant after multiple bowel movements. Applying zinc oxide cream to the anal area acts as a protective barrier. Since you will be spending several hours near a toilet, plan accordingly. Keep books, podcasts, or movies ready for the period when diarrhea sets in. Most people visit the restroom three to six times per hour during peak activity.
Electrolyte balance matters immensely. The prep washes out salts along with waste. Sipping electrolyte-replacement drinks throughout the day prevents cramping and maintains energy levels. Ensure these drinks are also clear liquid compliant. Planning the day off work is essential. Even if you feel fine physically, you will be tired. You also legally require an adult driver to take you home afterward, as sedation affects coordination for 24 hours.
What Comes After the Exam
Once the scope returns, recovery is usually quick. Most people resume normal eating once they feel hungry and can tolerate food. Your provider will discuss the findings. If the preparation was excellent, they likely saw every fold of the colon clearly. If visibility was compromised, they may advise an earlier repeat exam. Trust the process. The temporary discomfort of preparation outweighs the long-term benefit of catching cancer early by a massive margin.
Can I eat breakfast the morning of my colonoscopy?
No. You must stop all solid foods at least three hours before your scheduled time. For morning procedures, this usually means no breakfast at all. Stick to clear liquids until the cut-off point specified by your clinic, which is typically 10 AM for afternoon procedures.
Does the preparation cause permanent damage to digestion?
Not at all. The laxative induces temporary rapid transit to clear the colon. Once you return to a regular diet, your bowel function normalizes within 24 to 48 hours. Your body reabsorbs lost fluids quickly.
What if I cannot finish the entire laxative bottle?
If you feel nauseated, pause for 30 minutes, then try small sips again. Cold temperature helps. If you vomit excessively, contact your doctor immediately. They may provide alternative medication or adjust the timing. Partial cleansing still poses risks for missing polyps, so rescheduling might be safer.
Do I need to change my prescription medications?
Most daily medications continue as normal, taken with a small sip of water. Exceptions include diabetes medication and iron supplements, which require specific adjustments. Always ask your doctor for a tailored list before the day of the exam.
How do I know if my colon is clean enough?
The final output should be clear yellow or light liquid, similar to urine. Solid particles or dark colors indicate you need to continue drinking fluids. If it remains murky after finishing the prep, inform the triage nurse upon arrival.








8 Comments
just drink the water and dont worry about the rest 🙂
You really need to take this seriously!!! The cleansing agent tastes bad initially 😮😬. Chilling it helps immensely though 🥶❄️. You cannot rush the drinking schedule either ⏱️⚡. Split doses work far better than one sitting 🍽️👌. Hydration keeps your head from spinning too much 💧🧠. Clear liquids are non negotiable for the result 🚫🍔. Red fluids stain the lining terribly 🛑💉. Doctors miss spots when residue remains present 👀📉. We all know cancer screening saves lives daily ❤️🏥. Preparation quality dictates the detection rate significantly 📈✅. Polyps grow silently if left alone behind 🐌🚨. Comfort measures make the night manageable 😴🛁. Wet wipes protect sensitive skin effectively 🧻✨. Zinc cream prevents burning sensations nicely 🩹💊. Rest up so you do not feel weak later 😴🛌. Your health depends on diligence!! 😊💪
Glad you got through it safely 😊 definitely listen to the instructions closely 🤍
Your enthusiasm regarding bowel evacuation seems misplaced given the reality.
You need to understand why others share their experiences 😠 self preservation is moral duty here 😤
Life often requires us to swallow things we dislike for a greater good. Prevention is better than cure indeed 🌿
The medical advice provided is sound. Follow the timeline strictly for best results 🎯
A visceral journey through the digestive tract awaits the brave. Prepare your senses for the odyssey ahead!