Glaucoma: How to Spot It, Treat It, and Protect Your Vision
Glaucoma often sneaks up without pain and can steal sight before you notice. That sounds scary because many people only find out at a late stage. The good news: with the right checks and care, you can slow or stop vision loss. This page gives clear, practical steps — what to watch for, how doctors test for it, and what you can do every day to protect your eyes.
How you notice glaucoma
Most people don’t feel early glaucoma. That’s why regular eye checks matter. Common signs to watch for: patchy blind spots in side (peripheral) vision, tunnel vision in later stages, or sudden eye pain and blurred vision with nausea in acute cases. Ask yourself: can you see well to the side without turning your head? If not, mention it at your next eye exam.
Risk factors raise the chance of glaucoma: being over 60, family history, very high eye pressure, certain ethnicities (for example African or Latino ancestry), long-term steroid use, and conditions like diabetes. If any of these apply, tell your eye doctor and get tested more often.
Treatments and everyday steps
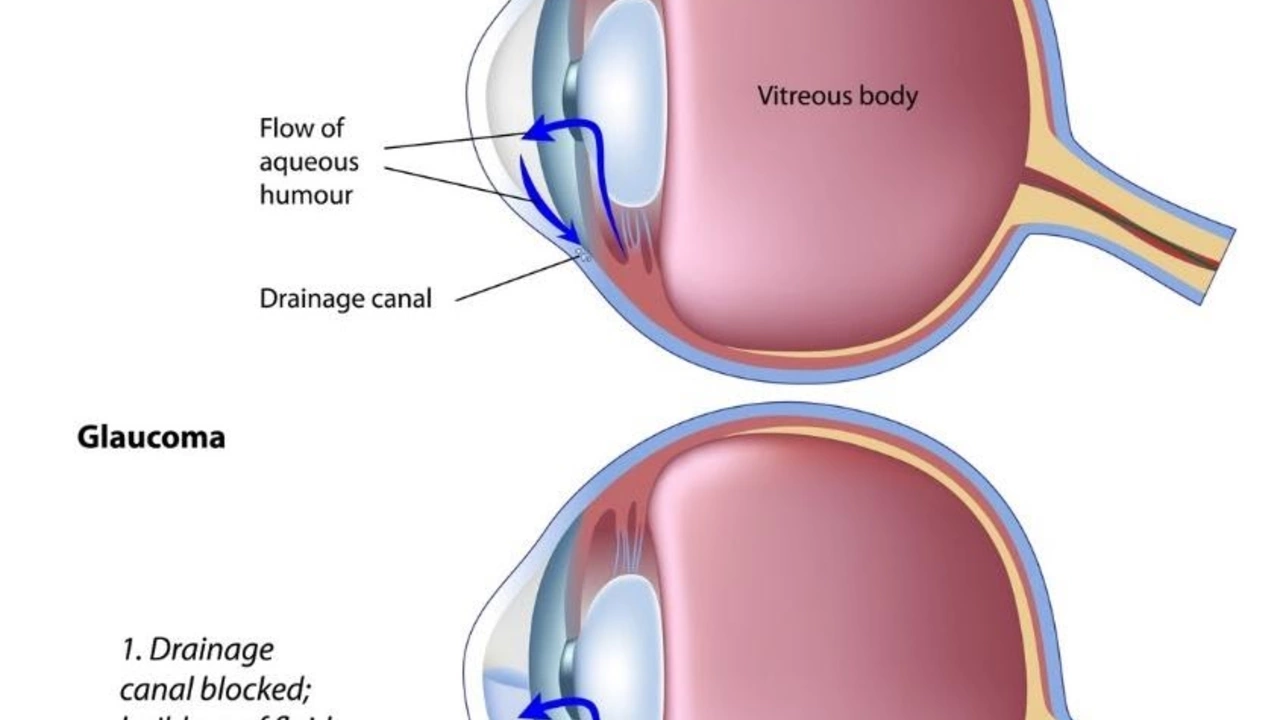
Treatment focuses on lowering pressure inside the eye to prevent further damage. Most people start with prescription eye drops that reduce fluid production or improve drainage. These need to be used regularly — missing doses lowers effectiveness. If drops don’t work well enough, laser procedures can help open blocked drainage channels. Surgery is another option when other steps don’t control pressure.
What you can do at home matters too. Take prescribed drops exactly as directed and keep all follow-up visits. Exercise moderately — brisk walking can help lower eye pressure for some people. Avoid smoking and manage blood sugar if you have diabetes. Don’t start or stop steroid medicines without checking with your doctor, because steroids can raise eye pressure.
Keep a personal record: date of diagnosis, medications, side effects, and pressure readings from visits. That makes conversations with specialists simpler and helps spot trends. If vision changes suddenly — increased blurriness, halos around lights, severe eye pain, or nausea — seek emergency care. Those signs may mean acute angle-closure glaucoma, which needs quick treatment.
Regular screening is the best prevention. Adults over 40 should ask about glaucoma testing at their routine eye exam; people at higher risk may need checks sooner and more often. Tests are painless and include measuring eye pressure, inspecting the drainage angle, and checking the optic nerve and peripheral vision.
You don’t have to accept vision loss as inevitable. With timely checks, consistent treatment, and simple lifestyle steps, most people keep useful vision for life. If you suspect any changes or you’re due for an eye exam, book one now and tell your doctor about your risk factors and any vision changes you've noticed.
Cabergoline and Glaucoma: A Potential Treatment Option
In my recent research, I delved into the potential of Cabergoline as a treatment option for glaucoma. Glaucoma, a leading cause of blindness, could possibly be treated with this medication, traditionally used for Parkinson's disease and hormonal disorders. Studies are showing promising results with Cabergoline reducing intraocular pressure, a key factor in glaucoma. However, more extensive research is needed to fully understand the drug's effectiveness and potential side effects. It's exciting to think we could be on the cusp of a new treatment option for this debilitating eye disease.
read more

